World Heart Day
The heart and blood vessels constitute the cardiovascular (circulatory) system. The heart pumps the blood to the lungs so it can pick up oxygen and then pumps oxygen-rich blood to the body. The blood circulating in this system delivers oxygen and nutrients to the tissues of the body and removes waste products (such as carbon dioxide) from the tissues.
The heart, a hollow muscular organ, is located in the center of the chest. The heart has two sides, right and left. The right and left sides of the heart each have an :
Atrium: Upper chamber that collects blood and pumps it to the lower chamber.
Ventricle: Lower chamber, which pumps blood out of the heart
To ensure that blood flows in only one direction, each ventricle has an "in" (inlet) valve and an "out" (outlet) valve.

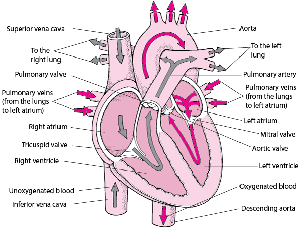
In the left ventricle, the inlet valve is the mitral valve, and the outlet valve is the aortic valve. In the right ventricle, the inlet valve is the tricuspid valve, and the outlet valve is the pulmonic (pulmonary) valve.
Each valve consists of flaps (cusps or leaflets), which open and close like one-way swinging doors. The mitral valve has two cusps. The other valves (tricuspid, aortic, and pulmonic) have three. The large inlet valves (mitral and tricuspid) have tethers—consisting of the papillary muscles and cords of tissue—which prevent the valves from swinging backward into the atria. If a papillary muscle is damaged (for example, by a heart attack), the valve may then swing backward and start leaking (called regurgitation). If a valve opening is narrowed (called stenosis), blood flow through the valve is reduced. Both leaking and narrowing may occur in the same valve.
The heartbeats are evidence that the heart is pumping , Each heartbeat has two parts:
Systole: During systole, the ventricles contract and pump blood out of the heart, and the atria relax and begin filling with blood again.
Diastole: During diastole, the ventricles relax and fill with blood. Then the atria contract, forcing more blood into the ventricles.
The contraction of the muscle fibers in the heart is very organized and highly controlled. Every heart muscle fiber does not contract at exactly the same time. Instead, the fibers contract in a sequence that best pumps blood out of each heart chamber. The contraction sequence is controlled by rhythmic electrical impulses (discharges) that flow through the heart in a precise manner along distinct pathways and at a controlled speed.
The impulses originate in the heart's natural pacemaker (the sinus or sinoatrial node—a small mass of tissue in the wall of the right atrium), which generates a tiny electrical current.
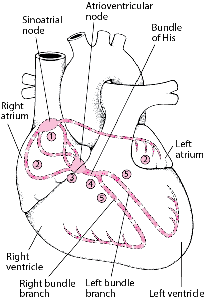
Tracing the Heart’s Electrical Pathway
The sinoatrial (sinus) node (1) initiates an electrical impulse that flows through the right and left atria (2), making them contract. When the electrical impulse reaches the atrioventricular node (3), it is delayed slightly. The impulse then travels down the bundle of His (4), which divides into the right bundle branch for the right ventricle (5) and the left bundle branch for the left ventricle (5). The impulse then spreads through the ventricles, making them contract.

The heart rate, or pulse, is the number of times the heart beats within a minute. The heart rate goes up when the body needs more oxygen (such as during exercise). The heart rate goes down when the body needs less oxygen (such as during rest).
The rate at which the sinus node sends out its impulses governs the heart rate. The sinus node has its own rate of sending out impulses. This rate can be modified by two opposing parts of the autonomic nervous system—one part speeds the heart rate up (the sympathetic division of the nervous system) and one slows it down (the parasympathetic division).
The sympathetic division : works through a network of nerves called the sympathetic plexus and through the hormones epinephrine (adrenaline) and norepinephrine (noradrenaline), which are released by the adrenal glands and the nerve endings.
The parasympathetic division : works through a single nerve—the vagus nerve—which releases the neurotransmitter acetylcholine.
The World Health organization noted that cardiovascular diseases are the leading causes of death worldwide, More deaths from these diseases than from any of the other causes of death.
World Heart Day aims to raise awareness of the risk factors that can lead to these diseases such as high blood pressure, high levels of sugar and cholesterol in the blood and smoking, Lack of physical activity and healthy balanced eating.
So how to protect yourself from heart disease :
Lifestyle and home remedies
Heart disease can be improved — or even prevented — by making certain lifestyle changes. The following changes are recommended to improve heart health :
Don't smoke. Smoking is a major risk factor for heart disease, especially atherosclerosis. Quitting is the best way to reduce the risk of heart disease and its complications. If you need help quitting, talk to your provider.
Eat healthy foods. Eat plenty of fruits, vegetables and whole grains. Limit sugar, salt and saturated fats.
Control blood pressure. Uncontrolled high blood pressure increases the risk of serious health problems. Get your blood pressure checked at least every two years if you're 18 and older. If you have risk factors for heart disease or are over age 40, you may need more-frequent checks. Ask your health care provider what blood pressure reading is best for you.
Get a cholesterol test. Ask your provider for a baseline cholesterol test when you're in your 20s and then at least every 4 to 6 years. You may need to start testing earlier if high cholesterol is in your family. You may need more-frequent checks if your test results aren't in a desirable range or you have risk factors for heart disease.
Manage diabetes. If you have diabetes, tight blood sugar control can help reduce the risk of heart disease.
Exercise.Physical activity helps you achieve and maintain a healthy weight. Regular exercise helps control diabetes, high cholesterol and high blood pressure — all risk factors for heart disease. With your provider's OK, aim for 30 to 60 minutes of physical activity most days of the week. Talk to your health care provider about the amount and type of exercise that's best for you.
Maintain a healthy weight. Being overweight increases the risk of heart disease. Talk with your care provider to set realistic goals for body mass index (BMI) and weight.
Manage stress.Find ways to help reduce emotional stress. Getting more exercise, practicing mindfulness and connecting with others in support groups are some ways to reduce and manage stress. If you have anxiety or depression, talk to your provider about strategies to help.
Practice good hygiene.Regularly wash your hands and brush and floss your teeth to keep yourself healthy.
Practice good sleep habits.Poor sleep may increase the risk of heart disease and other chronic conditions. Adults should aim to get 7 to 9 hours of sleep daily. Kids often need more. Go to bed and wake at the same time every day, including on weekends. If you have trouble sleeping, talk to your provider about strategies that might help.
The three major types of ECG are :
• resting ECG or standard ECG – you lie down for this type of ECG. No movement is allowed during the test, as electrical impulses from other muscles can interfere with the test. This type of ECG usually takes five to 10 minutes.

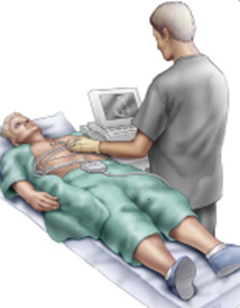
This can be done by our Biocare ECG devices
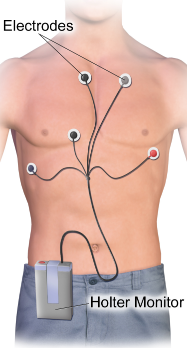
• ambulatory ECG or Holter – for an ambulatory ECG you wear a portable recording device for at least 24 hours. You are free to move around normally while the device is attached. A doctor may arrange this type of ECG if you have symptoms that are intermittent (stop-start) which may not show up on a resting ECG. Your doctor may also recommend an ambulatory ECG if you are recovering from heart attack, to ensure your heart is working properly. You may be asked to write down or record any symptoms you experience while wearing the device, including when they occur, so that your own experience can be compared with the ECG.

• exercise stress test/stress test – this type of ECG helps your doctor see how well your heart is working during physical activity. It involves having an ECG while you ride a stationary exercise bike or walk on a treadmill. This type of ECG takes about 15 to 30 minutes to complete. A stress test can also involve medicines, to understand their effects on the heart.

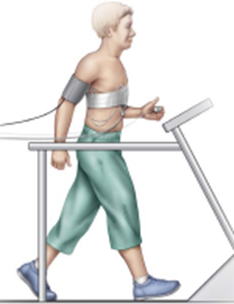
Having an ECG
An ECG is a simple test that usually doesn’t need any special preparation.
• You can eat and drink as normal before having an ECG (unless your doctor has advised otherwise).
• Always let your doctor know what medicines you are taking before you have an ECG.
• Let your doctor know if you have any allergies to adhesive tapes, as an adhesive is needed to attach the electrodes to the skin.
• You will need to remove your upper clothing so that electrodes can be attached to your chest, arms and legs. Wearing a separate top with trousers or a skirt can allow easy access to the chest. Underwire in a bra can interfere with the ECG reading – you may be asked to remove it before the test.
• An ECG works best when the skin is clean and dry, and free of oils and lotions. Sometimes the skin is shaved if necessary because hair prevents the electrodes from sticking properly to the skin.
Standard ECG device consists of 4 main parts :
1. Machine which consists of :
- - CPU port ( represents the brain and the heart of the device )
- - Colored screen which displays 12-leads before the printing.
- - Built-in battery which allows you to operate the device for 2 hours without power supply.
- - High quality printer
- - Partion in which we put the role of paper.
- - Keys which is easy to use.
- - Output for electricity cable
- - 2 USB
- - Internal memory
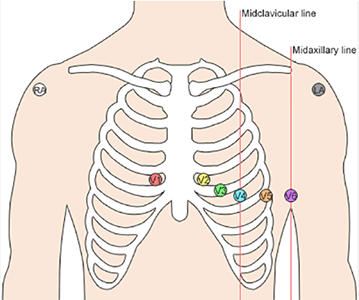
2. Bulb or chest electrodes consists of 6 electrodes which we put on the chest and the silver or potassium chloride gel will be applied to permit electron conduction from the skin to the wire and the ECG machine.

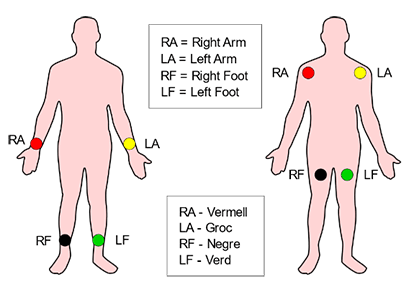
3. Clamp or limb electrodes consists of 4 reusable peripheral clamps , they have features that make them absolutely reliable during signal recording , the electrode metallic part is made of silver coated material allowing a safe and clear signal transmission, this clamps are attached in the limbs 2 of them are in right and left arm and the other 2 in the left leg and the right leg but this one called grounding or neutral electrode.

4. Patient cable or ECG cable which interface between electrodes and machine carries the electrical impulses to the machine CPU board to analysis and display the ECG complex.
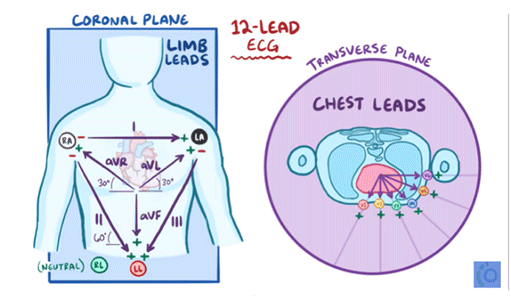
Standard ECG reads 12 Leads which get different views of the heart , make it easier to see exactly how the wave of depolarization moves through the heart.
12 Leads are grouped in 2 planes :
1) Horizontal plane group which are the Chest Leads
( V1 , V2 , V3 , V4 , V5 , V6 )
2) Frontal plane group which are the Limb Leads
( avL , avR , avF , Lead I , Lead II , Lead III )
- avL , avR , avF are unipolar leads and they called augmented leads , those come from the left arm , right arm and left foot.
- Lead I , Lead II , Lead III are bipolar limb electrodes recorded using two electrodes instead of one.
- Leads are displayed in the ECG paper , it can be in one channel , three channels like in Biocare ECG IE 300 Device , 6 channels , 12 channels like in Biocare ECG 1210.
The ECG paper consists of big squares and small squares , each big square consists of 25 small square and it measure heart electrical activity in 1 second.
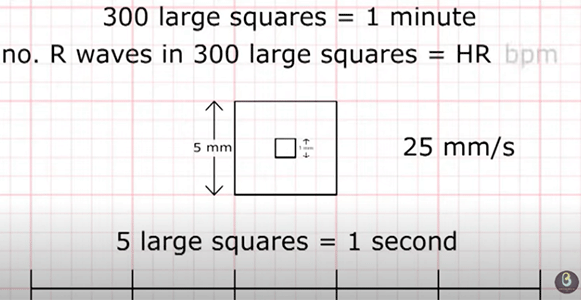
The horizontal axis of the paper represent duration , the vertical axis represent amplitude. So make sure that the device speed is set to 25 mm/sec
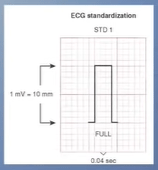
Don’t forget to take a look at standardization mark and make sure that it displays 2 big squares.

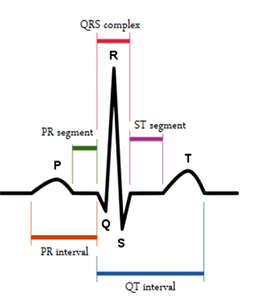
The device draw the heart electrical wave as it shown below and it called PQRST wave.

•https://www.mayoclinic.org/diseases-conditions/heart-disease/diagnosis-treatment/drc-20353124
• https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/ecg-test
• https://canberraheartrhythm.com.au/
•https://intermountainhealthcare.org/
•https://arabic.cnn.com/health/article/2020/09/29/who-world-heart-day-2020
•Biomedical Engineers TV







